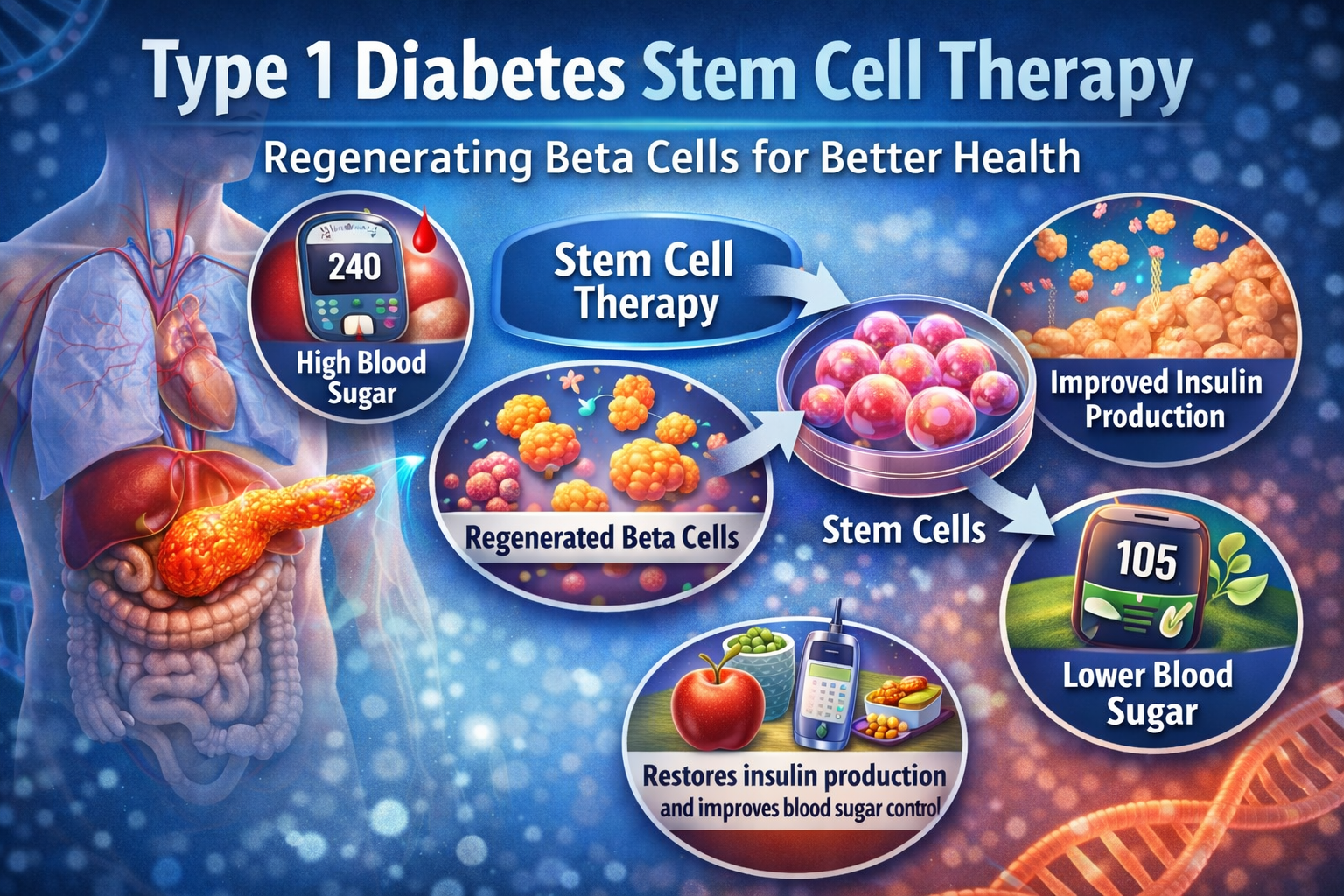
Type 1 Diabetes Stem Cell Therapy: A New Direction in Medical Research
Type 1 diabetes is a chronic condition that affects millions of people around the world. It occurs when the immune system mistakenly attacks and destroys insulin-producing beta cells in the pancreas. As a result, the body cannot produce enough insulin to regulate blood sugar levels. People living with this condition must rely on daily insulin injections or insulin pumps to manage their glucose levels. In recent years, researchers have been exploring innovative approaches that may change how this condition is treated in the future. One of the most promising developments is Type 1 Diabetes Stem Cell Therapy, which is gaining attention in the medical community.
Understanding Type 1 Diabetes
Before exploring new treatment possibilities, it is important to understand the condition itself. Type 1 diabetes is usually diagnosed in children, teenagers, or young adults, although it can develop at any age. The immune system targets and destroys the beta cells in the pancreas, which are responsible for producing insulin. Without insulin, glucose builds up in the bloodstream instead of entering the body’s cells for energy.
Common symptoms include increased thirst, frequent urination, fatigue, unexplained weight loss, and blurred vision. Managing the condition requires constant monitoring of blood sugar levels, a balanced diet, and insulin therapy. While current treatments help control symptoms, they do not restore the body’s natural ability to produce insulin.
What Are Stem Cells?
Stem cells are unique cells in the body that have the ability to develop into many different types of specialized cells. They also have the capability to divide and renew themselves over long periods. Because of these properties, stem cells are widely studied in regenerative medicine.
Scientists believe that stem cells may be used to repair or replace damaged tissues in various diseases. In the case of diabetes, researchers are studying whether these cells can be used to create new insulin-producing cells that function like healthy pancreatic beta cells.
How Stem Cell Therapy Works
The concept behind Type 1 Diabetes Stem Cell Therapy focuses on replacing the damaged or destroyed insulin-producing cells in the pancreas. Researchers attempt to grow new beta cells from stem cells in laboratory settings. These newly developed cells can then be transplanted into the patient’s body.
Once inside the body, the goal is for these cells to begin producing insulin naturally, helping regulate blood glucose levels. If successful, this approach could reduce or even eliminate the need for daily insulin injections.
Scientists are also exploring ways to protect newly transplanted cells from the immune system. Since the immune system originally attacked the patient’s beta cells, researchers are studying protective techniques such as encapsulation or immune-modulating therapies to help the new cells survive and function properly.
Types of Stem Cells Used in Research
Several types of stem cells are currently being studied for diabetes treatment. Each type offers different advantages and challenges.
Embryonic Stem Cells:
These cells are capable of transforming into almost any cell type in the body. Researchers can guide them to develop into insulin-producing beta cells. However, ethical considerations and immune rejection risks must be addressed.
Adult Stem Cells:
Adult stem cells are found in certain tissues of the body. Some studies suggest that they may be able to support tissue repair and help regulate immune responses.
Induced Pluripotent Stem Cells (iPSCs):
These cells are created by reprogramming adult cells, such as skin cells, into a stem-cell-like state. Scientists can then direct them to become beta cells. Because these cells can be created from a patient’s own tissues, they may reduce the risk of immune rejection.
Potential Benefits of Stem Cell Approaches
Research into Type 1 Diabetes Stem Cell Therapy offers several potential benefits that could improve the lives of people living with the condition.
One of the biggest advantages is the possibility of restoring the body’s natural insulin production. If new beta cells function correctly, patients may not need to rely on frequent insulin injections.
Another benefit is improved blood sugar stability. Natural insulin production can respond more precisely to changes in glucose levels, which may reduce the risk of severe highs and lows.
In addition, successful regenerative therapies may help reduce long-term complications related to diabetes. These complications can include nerve damage, kidney disease, eye problems, and cardiovascular issues.
Current Research and Clinical Trials
Medical researchers and biotechnology companies are actively studying stem cell-based treatments for diabetes. Several clinical trials are currently underway to evaluate safety, effectiveness, and long-term outcomes.
Some experimental treatments involve implanting stem-cell-derived beta cells inside small protective devices that allow insulin to pass through while shielding the cells from immune attacks. Other studies are focusing on immune therapies that help the body tolerate new insulin-producing cells.
While early results from some trials are promising, scientists emphasize that more research is required. Long-term safety and consistent effectiveness must be demonstrated before such therapies become widely available.
Challenges and Limitations
Although research into Type 1 Diabetes Stem Cell Therapy is encouraging, several challenges remain. One of the biggest obstacles is immune rejection. Because the immune system caused the disease in the first place, it may attack newly transplanted cells as well.
Another challenge involves ensuring that the transplanted cells function correctly and consistently over time. Scientists must also ensure that stem cell treatments do not lead to unwanted cell growth or other complications.
Cost and accessibility may also become important considerations in the future. Advanced regenerative treatments often require specialized laboratories and medical expertise, which can make them expensive during the early stages of development.
The Future of Diabetes Treatment
Despite these challenges, research in regenerative medicine continues to move forward. Advances in biotechnology, cell engineering, and immune therapy are helping scientists refine potential treatments.
In the coming years, improvements in Type 1 Diabetes Stem Cell Therapy may lead to safer and more effective approaches. Researchers are working to develop methods that combine cell replacement with immune system protection, which could significantly increase success rates.
If these efforts succeed, stem cell technology could transform how diabetes is treated. Instead of simply managing blood sugar levels, future therapies may address the underlying cause of the condition.
Conclusion
Type 1 diabetes remains a lifelong condition that requires careful management and continuous monitoring. However, scientific progress is opening new possibilities for more advanced treatments. Type 1 Diabetes Stem Cell Therapy represents one of the most exciting areas of research in modern medicine.
By focusing on regenerating insulin-producing cells and restoring the body’s natural glucose control, researchers hope to move closer to a long-term solution. Although further studies and clinical trials are needed, ongoing research continues to bring new hope to individuals and families affected by this condition.